Link to the Viruses Student Learning Guide
1. SARS-CoV-2? Covid-19? Key terms to know
The COVID-19 pandemic was caused by the SARS-CoV-2 virus. Let’s start by looking at what these acronyms stand for, as well as some associated terms.
- COVID-19 stands for Coronavirus Disease, 2019.
- Coronaviruses are a family of viruses that cause a variety of diseases of the respiratory system. Some coronaviruses cause the common cold. Others, such as MERS (Middle Eastern Respiratory Syndrome), cause much more serious diseases.
- SARS-CoV-2 stands for Severe Acute Respiratory Syndrome Coronavirus-2. According to Merriam Webster Online, the way to say the acronym is \ ˈsärz-kō-ˈvē-ˈtü \, with 4 syllables. It’s
- Severe because it can cause a serious illness.
- Acute because it comes on suddenly, as opposed to a chronic condition that you live with for a long time.
- Respiratory because it involves tissues in the lungs and upper respiratory system (nose, throat, etc.)
- A syndrome because there’s an array of symptoms.
- “2” because it’s the second coronavirus of this type to cause a pandemic. The first was called SARS-CoV, and it caused a pandemic that occurred in 2003 (one that was far smaller than the COVID-19 pandemic that started in last 2019).
How is a pandemic different from an epidemic? A pandemic is a disease that occurs in many countries or regions at the same time. The SARS outbreak of 2003 spread to 29 countries, affecting over 8000 people and resulting in 774 deaths (Source: CDC.gov). The COVID-19 pandemic has been much wider in scope, spreading to nearly every country on Earth, infecting over 632 million people, and causing over 6.6 million deaths. In the United States, there have been nearly 98 million infections and over 1,070,000 deaths (sources: John Hopkins Coronavirus Research Center and the WHO). Please email me when these numbers need updating.
Most infectious disease outbreaks are epidemics. An epidemic occurs in just one region or country, or even one area within a country. For example, the Ebola virus outbreak that occurred between 2014 and 2016 was mostly confined to Western Africa, making it an epidemic.
2. How SARS-CoV-2 spreads
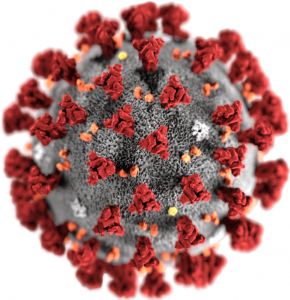
SARS-CoV-2 is spread by airborne transmission.
Like all viruses, SARS-CoV-2 is incredibly small. If you’re looking at this on a laptop computer, then the image on your right is about 5 centimeters in diameter. The actual virus is 100 nm (nanometers) in diameter. A nanometer is a billionth of a meter, so that’s 500,000 times smaller than what you’re seeing. Here are a few comparisons:
- A DNA molecule is about 2 nm wide. A single viral particle of SARS-Cov-2 is about 50 times wider than DNA.
- A strand of hair is about 80,000 nanometers thick. You could line up 800 particles of SARS-Cov-2 across a single strand of hair.
- According to The Engineering Toolbox, household dust is at least 50 nm in diameter, and could be up to 1000 times larger. So one viral particle is at most twice the size of a small particle of household dust.
When a person who’s infected with SARS-Cov-2 exhales, coughs or sneezes, they release viral particles and tiny droplets containing the virus into the air. These particles and droplets can float in the air, and they’ll be most highly concentrated in the area immediately around an infected person. If you spend time close to someone who’s infected with SARS-Cov-2, then you might breathe in some of the viral particles that that person is releasing into the air.
Wearing a mask can reduce your risk of inhaling the virus. The more effective the mask, the better the protection. Wearing a mask can also contain the spread of any virus that you might be infected with, so wearing a mask protects others.
In terms of protection from SARS-CoV-2, the best type of mask to wear is an N95, KN95, or FFP2 (the first two are used in North America, the latter in Europe). These provide better protection than surgical masks, which are, in turn, superior to cloth face coverings (see STAT news, a website that focuses on health and medicine).
3. What are the key structures in SARS-Cov-2?
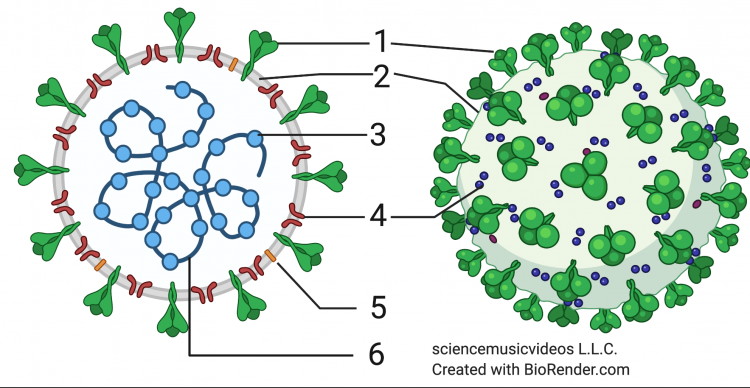 SARS-Cov-2 is an RNA virus. That means that RNA (number 6 in the diagram at left) makes up its genetic material. To review RNA’s structure, click here.
SARS-Cov-2 is an RNA virus. That means that RNA (number 6 in the diagram at left) makes up its genetic material. To review RNA’s structure, click here.
The RNA that makes up the SARS-CoV-2 genome consists of about 30,000 nucleotide bases. These bases code for 11 genes, which are expressed as 12 proteins.
The RNA is enclosed and protected by nucleocapsid proteins (at 3). The nucleocapsid proteins fit together to form a protective capsid (more easily seen in the image below from UK Research and Innovation).
In many viruses, such as the phage discussed in the previous tutorial, a genetic core and a capsid make up the entire structure of the virus. But in viruses that infect animals, there are often additional layers, and that’s also true of coronaviruses. In all coronaviruses, a lipid envelope (2) surrounds the nucleocapsid. This envelope is composed of a phospholipid bilayer, the same structure that makes up cell membranes. As we’ll see below, this phospholipid bilayer is “stolen” from the cells that the virus infects.
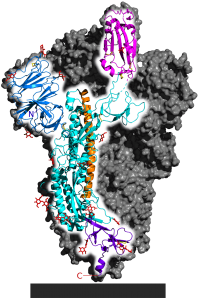
Embedded in the lipid envelope are several other proteins. The most prominent of these is the spike protein, at 1. These spikes create the corona (corona means “crown”) from which coronaviruses get their name. The spike protein is a quaternary protein, composed of 3 identical polypeptide subunits, one of which is shown in a highlighted, cartoon form in the diagram. As an AP Biology student, you should notice the many alpha helices that are part of the protein’s secondary structure, as well as the hairpin turns that are part of the tertiary protein structure.
The spike protein is important because it’s how the virus enters cells. The cyan-colored portion of the diagram (at the very top) is a receptor binding site. As we’ll see below, this part of the spike protein has evolved so that it can bind with a receptor on a cell in a person’s lungs or upper respiratory tract, inducing that cell to absorb the virus.
Another reason why the spike protein is important is that it’s the target of SARS-CoV-2 vaccines (which we explain in the next tutorial)
Two other proteins embedded in the virus’s membrane are the M protein (also known as the membrane protein, shown at 4) and the E protein (also known as the envelope protein, shown at 5).
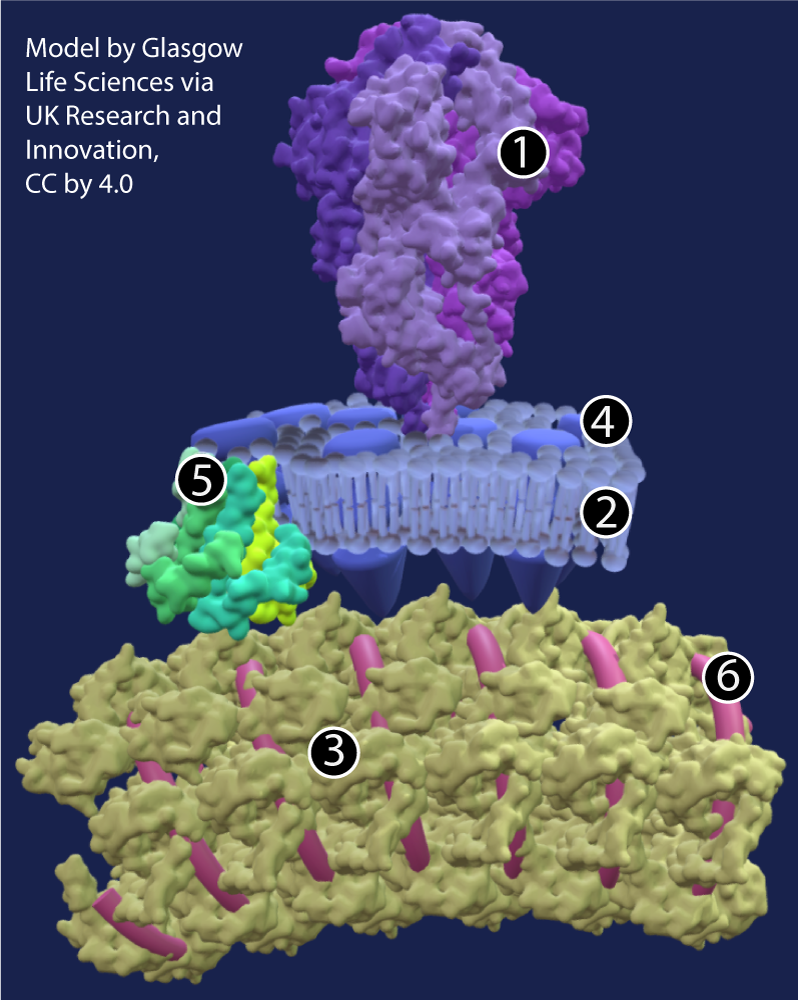
The image at right, from a 3-D model on “Getting to know the new coronavirus” by UK Research and Innovation, shows these structures in spectacular detail. Click the image to enlarge it.
Key:
- Spike protein
- phospholipid bilayer
- nucleocapsid protein
- Membrane protein
- Envelope protein
- RNA
4. SARS-CoV-2 Structure: Checking Understanding
Before delving deeper, let’s check for understanding.
[qwiz style=”width: 600px !important; min-height: 400px !important;” qrecord_id=”sciencemusicvideosMeister1961-SARS-CoV-2 Structure” random=”true”]
[h] SARS-CoV-2 Structure: Checking Understanding
[i]
[q] In the diagram below, the spike protein is at
[textentry single_char=”true”]
[c]ID E=[Qq]
[f]IEV4Y2VsbGVudC4gJiM4MjIwOzEmIzgyMjE7IGlzIHRoZSBzcGlrZSBwcm90ZWluLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgc3Bpa2UgcHJvdGVpbiBpcyB0aGUgbW9zdCBwcm9taW5lbnQsIGVhc2lseSBzZWVuIHByb3RlaW4gb24gdGhlIHZpcnVzJiM4MjE3O3Mgc3VyZmFjZS4=[Qq]
[q] In the diagram below, which part is made of phospholipids?
[textentry single_char=”true”]
[c]ID I=[Qq]
[f]IEV4Y2VsbGVudC4gJiM4MjIwOzImIzgyMjE7IGlzIHRoZSB2aXJhbCBlbnZlbG9wZSwgYW5kIGl0JiM4MjE3O3MgbWFkZSBvZiBwaG9zcGhvbGlwaWRzIChkZXJpdmVkIGZyb20gdGhlIGNlbGzCoCB0aGF0IHN5bnRoZXNpemVkIHRoZSB2aXJ1cyk=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBQaG9zcGhvbGlwaWRzIG1ha2UgdXAgdGhlIHZpcnVzJiM4MjE3OyBlbnZlbG9wZS4=[Qq]
[q] In the diagram below, the nucleocapsid is at
[textentry single_char=”true”]
[c]ID M=[Qq]
[f]IENvcnJlY3QuICYjODIyMDszJiM4MjIxOyBpcyB0aGUgbnVjbGVvY2Fwc2lkLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgbnVjbGVvY2Fwc2lkIHN1cnJvdW5kcyBhbmQgcHJvdGVjdHMgdGhlIHZpcnVzJiM4MjE3O3MgUk5BLg==[Qq]
[q] In the diagram below, the virus’s genetic material is shown at
[textentry single_char=”true”]
[c]ID Y=[Qq]
[f]IE5pY2Ugam9iLiAmIzgyMjA7NiYjODIyMTsgaXMgdGhlIHZpcnVzJiM4MjE3O3MgZ2VuZXRpYyBtYXRlcmlhbCAoUk5BKS4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgZ2VuZXRpYyBtYXRlcmlhbCBjb25zaXN0cyBvZiBhIGxvbmcgc3RyaW5nIG9mIFJOQS4gV2hpY2ggcGFydCBvZiB0aGUgZGlhZ3JhbSBjb3VsZCBiZSBkZXNjcmliZWQgYXMgYSAmIzgyMjA7bG9uZyBzdHJpbmc/JiM4MjIxOw==[Qq]
[q] In the diagram below, which part is made of RNA?
[textentry single_char=”true”]
[c]ID Y=[Qq]
[f]IEF3ZXNvbWUuICYjODIyMDs2JiM4MjIxOyBpcyB0aGUgdmlydXMmIzgyMTc7cyBnZW5ldGljIG1hdGVyaWFsLCB3aGljaCBpcyBtYWRlIG9mIFJOQS4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgZ2VuZXRpYyBtYXRlcmlhbCBjb25zaXN0cyBvZiBhIGxvbmcgc3RyaW5nIG9mIFJOQS4gV2hpY2ggcGFydCBvZiB0aGUgZGlhZ3JhbSBjb3VsZCBiZSBkZXNjcmliZWQgYXMgYSAmIzgyMjA7bG9uZyBzdHJpbmc/JiM4MjIxOw==[Qq]
[q] In the diagram below, the spike protein is at
[textentry single_char=”true”]
[c]ID E=[Qq]
[f]IE5pY2VseSBkb25lLiBUaGUgc3Bpa2UgcHJvdGVpbiBpcyBzaG93biBhdCAxLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgc3Bpa2UgcHJvdGVpbiBpcyBieSBmYXIgdGhlIG1vc3QgcHJvbWluZW50IHN0cnVjdHVyZSBvbiB0aGUgdmlydXMmIzgyMTc7cyBzdXJmYWNlLg==[Qq]
[q] In the diagram below, RNA is shown at
[textentry single_char=”true”]
[c]ID Y=[Qq]
[f]IEF3ZXNvbWUuIFRoZSB2aXJ1cyYjODIxNztzIFJOQSAod2hpY2ggbWFrZXMgdXAgaXRzIGdlbmV0aWMgbWF0ZXJpYWwpIGlzIHNob3duIGF0IDYu[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgc3Bpa2UgcHJvdGVpbiBpcyBieSBmYXIgdGhlIG1vc3QgcHJvbWluZW50IHN0cnVjdHVyZSBvbiB0aGUgdmlydXMmIzgyMTc7cyBzdXJmYWNlLg==[Qq]
[q] In the diagram below, the nucleocapsid is shown at
[textentry single_char=”true”]
[c]ID M=[Qq]
[f]IFRlcnJpZmljLiBUaGUgbnVjbGVvY2Fwc2lkIGNvbnNpc3RzIG9mIHByb3RlaW5zIHRoYXQgY292ZXIgYW5kIHByb3RlY3QgdGhlIHZpcnVzJiM4MjE3O3MgUk5BLiBJdCYjODIxNztzIHNob3duIGF0IDMu[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgc3Bpa2UgcHJvdGVpbiBpcyBieSBmYXIgdGhlIG1vc3QgcHJvbWluZW50IHN0cnVjdHVyZSBvbiB0aGUgdmlydXMmIzgyMTc7cyBzdXJmYWNlLg==[Qq]
[q] In the diagram below, which part was stolen from the internal and external membranes of the cell that was used to make the virus?
[textentry single_char=”true”]
[c]ID I=[Qq]
[f]IENvcnJlY3QuIFRoZSB2aXJhbCBtZW1icmFuZSBpcyBjb21wb3NlZCBvZiBwaG9zcGhvbGlwaWRzIHRoYXQgd2VyZSBvbmNlIHBhcnQgb2YgYSBodW1hbiBjZWxsJiM4MjE3O3MgZW5kb21lbWJyYW5lIHN5c3RlbSwgb3IgaXRzIG91dGVyIG1lbWJyYW5lLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGlzIHBhcnQgaXMgY29tcG9zZWQgb2YgcGhvc3Bob2xpcGlkcyB0aGF0IGZvcm0gYSBiaWxheWVyLiBXaGljaCBzdHJ1Y3R1cmUgY291bGQgYmUgYSBiaWxheWVyIChjb21wb3NlZCBvZiB0d28gbGF5ZXJzKT8=[Qq]
[q] The “A” in SARS stands for [hangman]
[c]IGFjdXRl[Qq]
[q] A disease outbreak that occurs in many places at the same time is known as a [hangman]. By contrast, a disease that occurs in just one location is known as a(n) [hangman].
[c]IHBhbmRlbWlj[Qq]
[c]IGVwaWRlbWlj[Qq]
[q] In the reading above, you learned that a single SARS-CoV-2 particle is about 50 times wider than a molecule of [hangman] but much smaller than a particle of [hangman] floating in the air. And because the virus can float, it’s very important to protect yourself and others by wearing a [hangman].
[c]IEROQQ==[Qq]
[c]IGR1c3Q=[Qq]
[c]bWFzaw==[Qq]
[q]The spike protein is a [hangman]-level protein, consisting of 3 polypeptide chains.
In the image at left, you can see a few long alpha helices, which is a [hangman] protein structure.
[c]cXVhdGVybmFyeQ==[Qq]
[c]c2Vjb25kYXJ5[Qq]
[/qwiz]
5. How does SARS-CoV-2 Infect Cells?
To get infected by SARS-CoV-2, you have to breathe it in. According to the U.S. CDC (Centers for Disease Control):
COVID-19 spreads between people who are in close contact (within about 6 feet) through respiratory droplets, created when someone talks, coughs, or sneezes.
Once you breathe it in, the virus can come into contact with the cells in your respiratory system. As we’ve seen in the previous tutorial in this module, viruses take control of cells and convert them into virus factories. The image below shows how this works for SARS-CoV-2.
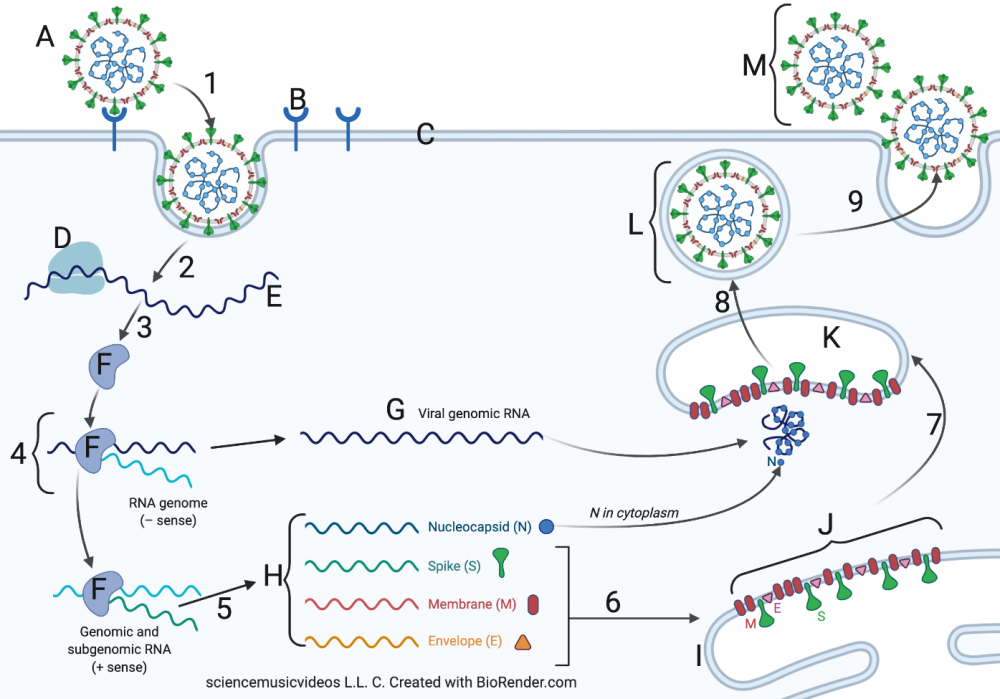
Suggestion: Keep the image in view as you scroll the text below.
- Steps 1 and 2: Viral binding and entry, Release of viral RNA. The infection cycle begins when the spike protein on SARS-CoV-2 binds with the ACE2 protein (at B) on the membrane (C) of an epithelial cell in the respiratory system. Epithelial cells form the outer lining of tissues in the nasal cavity, the lungs, and the blood vessels. “ACE2” stands for angiotensin-converting enzyme 2. ACE2’s function is to modify a hormone called angiotensin, which is used to regulate blood pressure.
During the evolution of SARS-CoV-2, its spike evolved in such a way that its shape became complementary to the shape of ACE2. That essentially made ACE2 into a receptor for SARS-CoV-2. The binding of the spike protein with ACE2 induces the cell to carry out something very similar to receptor-mediated endocytosis. In this process, the binding of a ligand with a receptor causes the cell membrane to buckle inward, bringing in whatever has bound to the receptor. The result, shown at 2, is that the RNA of SARS-CoV-2 can enter its new host. - Step 3: Synthesis of viral RNA polymerase. SARS-CoV-2 is what’s called a positive sense RNA virus. That means that its RNA can serve as messenger RNA for the ribosomes of an infected cell. One of these ribosomes is shown at “D.” Note that this ribosome “belongs” to the infected cell. If you were infected, it would be one of your ribosomes, in one of your epithelial cells. This ribosome reads the virus’s RNA message and makes a protein that’s unique to RNA viruses: RNA-dependent RNA Polymerase, also known as RNA replicase (shown at “F”). RNA replicase uses RNA as a template to synthesize a complementary strand of RNA. Note that while only one RNA replicase is shown in the diagram above, many are synthesized.
- Step 4: Replication of Genomic RNA. When RNA replicase synthesizes new RNA, that new strand is synthesized as minus RNA: it’s the complement of the original positive strand. In step 4, RNA replicase uses the minus RNA as a template to synthesize complementary RNA (at “G”). That strand of RNA is a replica of the 30,000 base RNA that makes up the virus’s genetic material (its genome). Later, in step 8, that genomic RNA will be incorporated into a new virus particle.
- Step 5: Replication of Structural RNAs. The genome of all coronaviruses consists of a variety of structural genes that code for viral proteins, including the spike protein, nucleocapsid protein, and other proteins discussed above. In step 5, RNA replicase creates copies of the mRNA for each of these proteins. These mRNAs are shown at “H.”
- Step 6: Translation of viral proteins. In step 6, ribosomes (not shown) translate these viral mRNAs at “H” into viral proteins (shown at “J”). These proteins are inserted into the endoplasmic reticulum (at “I”).
- Steps 7 and 8: Budding of vesicles from the ER; creation of new viruses. In step 7, vesicles with viral proteins bud off from the ER. In the cytoplasm, these vesicles combine with genomic RNA. With all required parts present, new viruses (“L”) are assembled (step 8).
- Step 9: Exocytosis and release of new viral particles. The newly formed virus at “L” is encased in a vesicle. In step 9 that vesicle fuses with the cell’s membrane (at “C”). This releases new viruses from the cell (shown at “M”). This virus may go on to infect other cells within the same person, worsening the infection. Alternatively, all it takes is for the infected person to exhale, speak, sing, cough, or sneeze to move that virus (along with many other viruses) outside of his or her body. If another person inhales those virus particles, the infection cycle can start again within his or her respiratory system.
6. Checking Understanding: The SARS-CoV-2 infection cycle
That’s a lot of detail. Let’s consolidate what you’ve learned with some interaction.
[h] SARS-CoV-2 Infection Cycle
[i] A Biohaiku
Coronavirus
Smaller than dust in the air
Remember your mask!
[q] In the diagram below, what letter or number represents a ribosome?
[textentry single_char=”true”]
[c]IE Q=[Qq]
[f]IEV4Y2VsbGVudCEgJiM4MjIwO0QmIzgyMjE7IHJlcHJlc2VudHMgYSByaWJvc29tZS4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IFNvcnJ5LCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBSaWJvc29tZXMgdHJhbnNsYXRlIG1STkEgaW50byBwcm90ZWluLiBXaGF0IGxldHRlciByZXByZXNlbnRzIFNBUlMtQ29WLTIgUk5BPw==[Qq]
[q] In the diagram below, the ACE2 protein is represented by which letter?
[textentry single_char=”true”]
[c]IE I=[Qq]
[f]IEZhYnVsb3VzISAmIzgyMjA7QiYjODIyMTsgcmVwcmVzZW50cyB0aGUgQUNFMiBwcm90ZWluLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlIGFyZSB0d28gaGludHMuIDEpIEFDRTIgaXMgYSByZWNlcHRvciBmb3IgYSBob3Jtb25lIGZvdW5kIG9uIHRoZSBtZW1icmFuZSBvZiBodW1hbiBlcGl0aGVsaWFsIGNlbGxzLiAyKSBUaGUgc3Bpa2UgcHJvdGVpbiBvbiBjb3JvbmF2aXJ1c2VzIGJpbmRzIHdpdGggQUNFMi4=[Qq]
[q] In the diagram below, RNA replicase is represented by
[textentry single_char=”true”]
[c]IE Y=[Qq]
[f]IE5pY2Ugam9iISAmIzgyMjA7RiYjODIyMTsgcmVwcmVzZW50cyBSTkEgcmVwbGljYXNlLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBSTkEgcmVwbGljYXNlIHJlcGxpY2F0ZXMgUk5BLiBGaW5kIHNvbWV0aGluZyB0aGF0IGxvb2tzIGxpa2UgaXQmIzgyMTc7cyB0YWtpbmcgUk5BIGFuZCBtYWtpbmcgY29waWVzIG9mIGl0Lg==[Qq]
[q] In the diagram below, which letter represents viral proteins in the endoplasmic reticulum before they’ve been assembled into new viruses?
[textentry single_char=”true”]
[c]IE o=[Qq]
[f]IEF3ZXNvbWUhICYjODIyMDtKJiM4MjIxOyByZXByZXNlbnRzIHZpcmFsIHByb3RlaW5zICYjODIyMDt3YWl0aW5nJiM4MjIxOyB0byBiZSBpbmNvcnBvcmF0ZWQgaW50byBuZXcgdmlydXNlcy4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IFNvcnJ5LCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGVzZSBwcm90ZWlucyBhcmUgd2FpdGluZyBpbiB0aGUgZW5kb3BsYXNtaWMgcmV0aWN1bHVtLCB3aGljaCBpcyBwYXJ0IG9mIGFuIGludGVybmFsIHNlcmllcyBvZiBtZW1icmFuZXMuIEZpbmQgc29tZXRoaW5nIGluc2lkZSB0aGUgY2VsbCB0aGF0IGxvb2tzIGxpa2UgaXQmIzgyMTc7cyBtYWRlIG9mIG1lbWJyYW5lLCBhbmQgeW91JiM4MjE3O2xsIGJlIG9uIHlvdXIgd2F5Lg==[Qq]
[q] In the diagram below, what number shows the formation of new viruses?
[textentry single_char=”true”]
[c]ID g=[Qq]
[f]IEF3ZXNvbWUhICYjODIyMDs4JiM4MjIxOyByZXByZXNlbnRzIHRoZSBwcm9jZXNzIG9mIHZpcnVzIGZvcm1hdGlvbi4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBBc3NlbWJseSBoYXBwZW5zIGltbWVkaWF0ZWx5IGJlZm9yZSB0aGUgbmV3bHkgYXNzZW1ibGVkIHZpcnVzZXMgbGVhdmUgdGhlIGNlbGwu[Qq]
[q] In the diagram below, what number shows the components of a new virus being brought together inside a vesicle? Note: this vesicle is more correctly referred to as the ERGIC (the ER-Golgi intermediate compartment).
[textentry single_char=”true”]
[c]ID c=[Qq]
[f]IFRlcnJpZmljISBTdGVwICYjODIyMDs3JiM4MjIxOyBzaG93cyBhbGwgdmlyYWwgY29tcG9uZW50cyBiZWluZyBicm91Z2h0IHRvZ2V0aGVyIGluIGEgdmVzaWNsZS4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IFNvcnJ5LCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBGaW5kIGEgc3RlcCB3aGVyZSB0aGUgdmlydXMmIzgyMTc7cyBnZW5ldGljIG1hdGVyaWFsIGFuZCBwcm90ZWlucyBhcmUgYWxsIGJlaW5nIGNvbWJpbmVkIGludG8gb25lICYjODIyMDtidWJibGUmIzgyMjE7IG9mIG1lbWJyYW5lLg==[Qq]
[q] In the diagram below, which number shows spike protein binding, followed by receptor-mediated endocytosis?
[textentry single_char=”true”]
[c]ID E=[Qq]
[f]IEdvb2Qgd29yayEgSW4gc3RlcCAmIzgyMjA7MSwmIzgyMjE7IHRoZSB2aXJ1cyBpcyBiaW5kaW5nIHdpdGggdGhlIEFDRTIgcHJvdGVpbi4gVGhpcyBpbmR1Y2VzIHRoZSBtZW1icmFuZSB0byBicmluZyB0aGUgdmlydXMmIzgyMTc7cyBjb250ZW50cyBpbnRvIHRoZSBjZWxsLiBJdCYjODIxNztzIHJlY2VwdG9yLW1lZGlhdGVkIGVuZG9jeXRvc2lzIChidXQgYSBraW5kIHRoYXQmIzgyMTc7cyBkaXNhc3Ryb3VzIGZvciB0aGUgY2VsbCku[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBGaW5kIGEgc3RlcCBpbiB3aGljaCBhIHJlY2VwdG9yIGJpbmRzIHdpdGggc29tZXRoaW5nLCBjYXVzaW5nIHRoZSBtZW1icmFuZSB0byBwaW5jaCBpbiBhbmQgYnJpbmcgc29tZXRoaW5nIGludG8gdGhlIGNlbGwu[Qq]
[q] In the diagram below, which number represents exocytosis?
[textentry single_char=”true”]
[c]ID k=[Qq]
[f]IE5pY2UhIEluIHN0ZXAgJiM4MjIwOzksJiM4MjIxOyB0aGUgdmlydXMgaXMgZXhwb3J0ZWQgZnJvbSB0aGUgY2VsbCwgYSBwcm9jZXNzIGFsc28ga25vd24gYXMgZXhvY3l0b3Npcy4=[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLg==[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiAmIzgyMjA7RXhvY3l0b3NpcyYjODIyMTsgbWVhbnMgJiM4MjIwO2V4cG9ydCBmcm9tIHRoZSBjZWxsLiYjODIyMTs=[Qq]
[q] In the diagram below, what letter represents the endoplasmic reticulum?
[textentry single_char=”true”]
[c]IE k=[Qq]
[f]IE5pY2UhICYjODIyMDtJJiM4MjIxOyByZXByZXNlbnRzIHRoZSBlbmRvcGxhc21pYyByZXRpY3VsdW0u[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[f]IE5vLCB0aGF0JiM4MjE3O3Mgbm90IGNvcnJlY3Qu[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgZW5kb3BsYXNtaWMgcmV0aWN1bHVtIGNvbnNpc3RzIG9mIGludGVybmFsIG1lbWJyYW5lcy4gV2hpY2ggcGFydCBjb3VsZCBiZSBhbiBpbnRlcm5hbCBtZW1icmFuZT8=[Qq]
[q] In the diagram below, letter D represents a [hangman], letter E represents [hangman], and letter F represents an enzyme called [hangman].
[c]IHJpYm9zb21l[Qq]
[c]IFJOQQ==[Qq]
[c]IHJlcGxpY2FzZQ==[Qq]
[q] In the diagram below, “G” is labeled as “viral genomic RNA.” By contrast, “H” represents RNAs that code for viral [hangman].
[c]IHByb3RlaW5z[Qq]
[/qwiz]
7. How does SARS-CoV-2 cause disease?
The severity of disease caused by SARS-CoV-2 varies widely. About 25% of those who become infected show few or no symptoms at all (PLOS Medicine, JAMA). While that sounds great, asymptomatic people (without symptoms) are still producing and exhaling the virus, enabling it to spread to others. In fact, the transmission of the disease from asymptomatic people might be a major driver behind the spread of the pandemic. (healthline.com). That’s one of the most important reasons for wearing masks. Masks help people from spreading the disease to others.
In most other cases (Centers for Disease Control) the most common symptoms of COVID-19 are similar to those associated with other respiratory infections: fever, coughing, muscle aches, sore throat, and congestion. One symptom unique to COVID-19 — experienced by about 80% of people who get infected — is loss of taste and/or smell. If you’re interested in learning more about that, read this article in Scientific American. The link will open in a new browser tab.
In a small proportion of patients, the disease can become severe. While this can happen to anyone, serious COVID-19 disease is most likely found in people who
- are older;
- have underlying health problems like high blood pressure, diabetes, chronic lung disease, or heart disease;
- are immunosuppressed (which means that their immune function is reduced).
To learn more about risk factors, please read this article. The link will open in a new browser tab.
In those with more serious disease, the effects of SARS-CoV-2 are mostly — but not entirely — seen in the lungs. In these cases, the virus might be
- Directly damaging cells in the lungs.
- Causing an immune response that leads to too much inflammation. Inflammation involves the release of fluid and pus into infected tissues. While that can normally help beat back an infection, too much inflammation can cause fluid to over-accumulate in the lungs, a condition that’s known as pneumonia. Pneumonia impairs a patient’s ability to absorb oxygen into their blood, and low blood oxygen levels are a sign of serious COVID-19.
- Causing blood clots in the lung, which can further damage lung tissue.
Because SARS-Cov-2 affects the tissue lining the circulatory system, the effects of the virus can be seen throughout the body. These effects include:
- kidney failure and kidney disease.
- damage to the heart and cardiovascular system.
To learn more about COVID-19, please consult this Wikipedia article (the link takes you to the disease section).
Finally, what’s above focuses on acute COVID-19 disease: what happens in the days and first few weeks following infection. However, a significant percentage of people who become infected with SARS-CoV-2 develop what’s called “long COVID.” This is an array of lingering symptoms that can persist long after the infection subsides. To learn more about long COVID, please use the links below.
- What Doctors Wish Patients Knew about Long COVID (from the American Medical Association)
- Post-COVID Conditions (from the Centers for Disease Control)
8. How do mRNA vaccines work?
Note: In the age of COVID, understanding immunity is a key part of scientific literacy. If you want to learn about the details of the immune system, you can do so through this Learn-Biology.com module. If you don’t have time for that, what’s below will give you enough background to understand mRNA vaccines: the most widely used type of vaccine against SARS-CoV-2.
When a person gets infected with a virus, their immune system launches a counterattack. That counterattack has many components, including
-
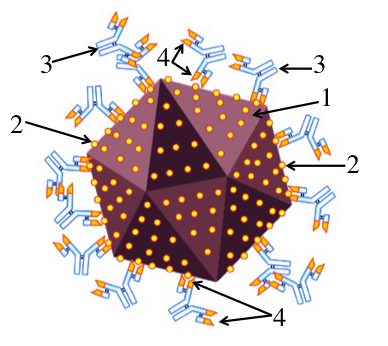
Antibodies (3) binding to and neutralizing a virus (1) Antibodies: Antibodies are proteins that bind with a virus. That neutralizes the virus and keeps it from entering and taking over cells.
- Killer T cells: These cells, also known as cytotoxic T cells, can find body cells that have been infected with the virus. The Killer T cells will kill these infected cells, keeping them from producing more viruses.
After the viral infection has been vanquished, you’ll develop immunity to that same virus. Immunity is based on
- Antibodies that continue to circulate in your bloodstream, which you’ll have for months following the initial infection.
- Memory cells. Memory cells are cells that your immune system creates following a successful counterattack against a virus (or any other pathogen). On a molecular level, memory cells “remember” the defeated virus, and wait in your lymph nodes, ready to counterattack if that same pathogen ever infects you again. The next time your body encounters that pathogen, your memory cells will quickly create antibodies and Killer T cells: so quickly that you’ll beat back the pathogen before you experience any symptoms.
A vaccine is a substance introduced into the body that trains your immune system to fight off a specific pathogen. Traditional vaccines (the ones we get as children against diseases like measles, mumps, polio, etc.) work by injecting either a weakened version of the virus, dead virus particles, or a small piece of that virus (usually a viral protein) into your body. What gets injected acts as an antigen, an “antibody generator.” In response to the antigen, your immune system creates antibodies and memory cells. This gives you immunity. If your body encounters that virus, you’ll quickly produce enough antibodies, killer T cells, and other immune system components to fight that virus off.
Vaccines have been in use for over 200 years. They prevent diseases that once caused millions of deaths (particularly among children) each year.
A variety of vaccines have been developed to provide us with immunity to SARS-CoV-2. You can learn more about these vaccines on this page on the NY Times website. For two reasons, I’m going to focus on one type of vaccine: mRNA vaccines. The first reason is that the way that mRNA vaccines work is particularly relevant to a college or AP-level Biology course. The second reason is that two leading vaccines used to protect against SARS-CoV-2 — the ones produced by the biotechnology companies Pfizer and Moderna — are mRNA vaccines. When you got vaccinated, these were most likely the vaccines that you received.
There are a few big ideas behind these mRNA vaccines:
- Unlike traditional vaccines, mRNA vaccines don’t use weakened or killed viruses (or even viral proteins) to elicit an immune response. Instead, they use a short segment of the virus’s mRNA. The mRNA used in the Pfizer and Moderna vaccines is a slightly modified version of the mRNA for the spike protein.
- Once injected, this mRNA goes into some of your cells, which start to produce the SARS-CoV-2 spike protein. The spike protein gets displayed on the membranes of these cells and is recognized by cells in the immune system.
- Recognition of the spike protein activates your immune system to learn how to recognize and fight off the SARS-CoV-2 virus.
Here’s some more detail about how mRNA vaccines work.
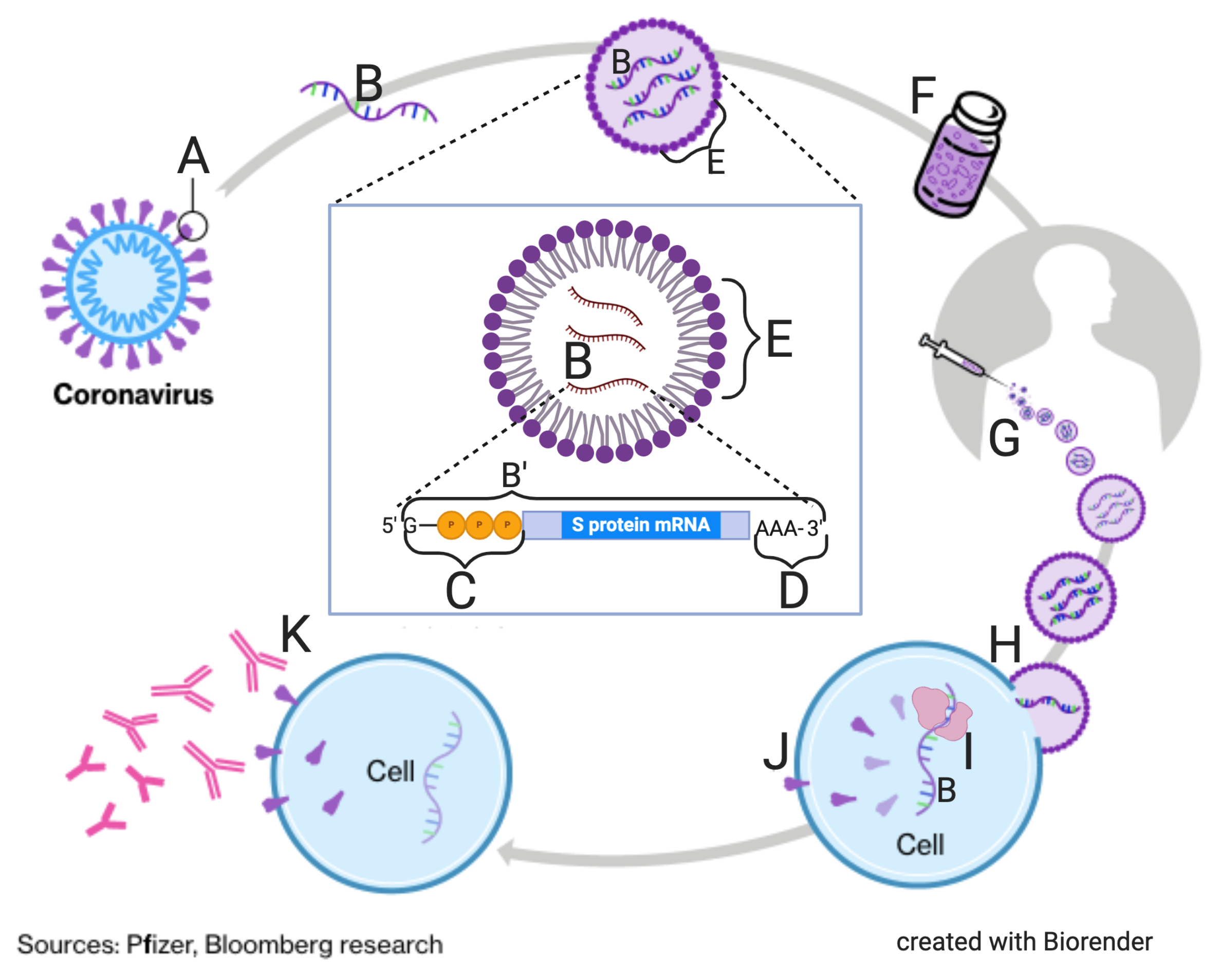 In the diagram to your left, “A” represents the spike protein of SARS-CoV-2. That protein was coded for by one of the protein-coding genes in the SARS-CoV-2 genome. “B” shows the RNA for that spike-protein-coding gene.
In the diagram to your left, “A” represents the spike protein of SARS-CoV-2. That protein was coded for by one of the protein-coding genes in the SARS-CoV-2 genome. “B” shows the RNA for that spike-protein-coding gene.
To make an mRNA vaccine, that mRNA is isolated, and modified in such a way that it’s ready for translation by a ribosome. This modification includes the addition of a 5′ GTP cap and a poly-A tail. Both of these modifications need to be engineered into the structure of an mRNA vaccine so that the mRNA can be translated by your ribosomes.
You can see this ready-to-translate mRNA shown at B’ in the large callout in the center of the image. At “C,” to the left of the S-protein mRNA sequence is a 5′ GTP cap. To the right, at the 3′ end of the mRNA is a poly-A tail (shown at “D”). The 5′ cap and the poly-A tail both serve to protect the mRNA from degradation by enzymes in the cytoplasm, giving the mRNA a long enough lifespan so that it can be translated by your cells.
Surrounding the mRNA is a lipid envelope, at E. This lipid envelope is what enables the viral mRNA to survive its trip through the bloodstream and enter a human cell.
Unlike DNA, which is a stable, tough molecule, mRNA is fragile. So is the lipid envelope. As a result, mRNA vaccines require ultra-cold storage. The Pfizer vaccine needs to be stored at -70° C. That requires a special freezer (much colder than the one you have in your kitchen). Moderna’s formulation is slightly less fragile, but still needs to be stored at -20° C (which is about the temperature of a kitchen freezer).
“F” shows a vaccine vial. Millions of these vials have been distributed around the U.S. (or any country where the public is getting vaccinated). “G” shows a hypodermic needle. A physician, nurse, or other trained technician injects you with the vaccine. The vaccine will float around in your bloodstream until it encounters one of your cells.
This encounter is shown at H. Your cell membranes are composed of lipids, and since lipids dissolve in lipids, the lipid envelope of the vaccine will fuse with your cells, dumping the viral mRNA inside.
Once inside your cells, the viral mRNA will be treated like any other mRNA. A ribosome (at “I”) will come along and read the viral mRNA. The result will be the production of the SARS-CoV-2 spike protein (at “J”). These proteins will then make their way to the surface of your cells.
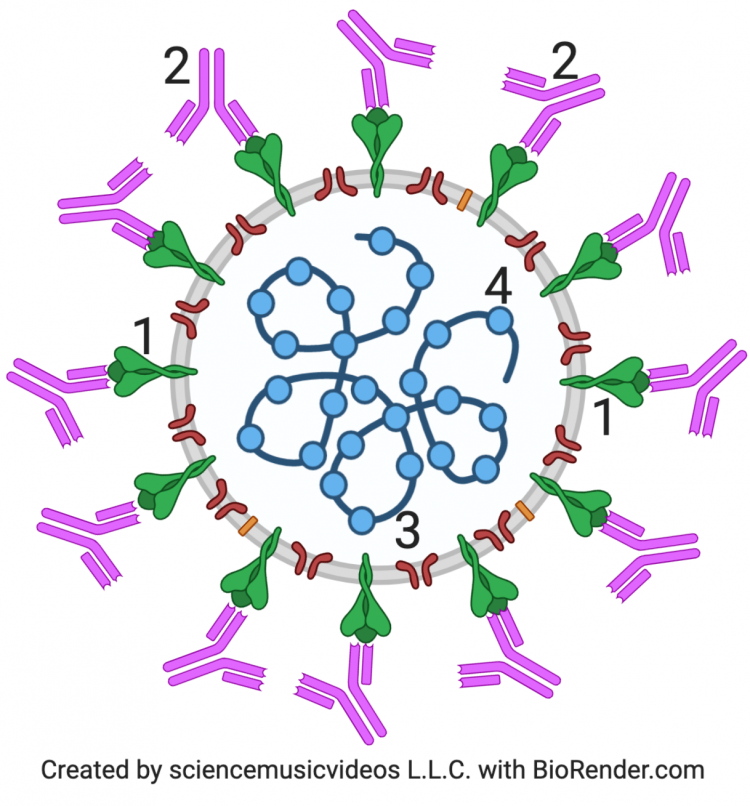 At this point, I’m leaving out many steps. The key point, however, is that your immune system will identify this protein as an antigen. And once that happens, your immune system will be able to produce antibodies that will bind to the spike protein on the surface of SARS-CoV-2, as shown on the left. The antibodies are shown at 2. They’re binding to viral spike proteins, shown at 1. And once they do, the virus can no longer infect human cells. It’s been neutralized.
At this point, I’m leaving out many steps. The key point, however, is that your immune system will identify this protein as an antigen. And once that happens, your immune system will be able to produce antibodies that will bind to the spike protein on the surface of SARS-CoV-2, as shown on the left. The antibodies are shown at 2. They’re binding to viral spike proteins, shown at 1. And once they do, the virus can no longer infect human cells. It’s been neutralized.
When your body knows how to do this, you have immunity. And thanks to mRNA vaccines you can get immunity without having to experience the symptoms associated with COVID-19.
9. Covid-19 disease and mRNA vaccines: Checking Understanding
[qwiz qrecord_id=”sciencemusicvideosMeister1961-COVID-19 Disease and mRNA Vaccines” random=”true”]
[h]Quiz: Covid-19 disease and mRNA vaccines
[i]
[q multiple_choice=”true”] True or false: if you don’t have any symptoms associated with COVID-19 (such as a runny nose or cough), you can’t spread the disease to others.
[c]IFRydWU=[Qq]
[f]IFNvcnJ5LiBUaGF0JiM4MjE3O3MgaW5jb3JyZWN0LiBNYW55IHBlb3BsZSB3aG8gZ2V0IGluZmVjdGVkIHdpdGggU0FSUy1Db1YtMiBhcmUgYXN5bXB0b21hdGljLCBidXQgdGhleSBjYW4gc3RpbGwgcHJvZHVjZSB0aGUgdmlydXMgYW5kIHNwcmVhZCBpdCB0byBvdGhlcnMuwqA=[Qq]
[c]IEZh bHNl[Qq]
[f]IENvcnJlY3QhwqA=TWFueSBwZW9wbGUgd2hvIGdldCBpbmZlY3RlZCB3aXRoIFNBUlMtQ29WLTIgYXJlIGFzeW1wdG9tYXRpYywgYnV0IHRoZXkgY2FuIHN0aWxsIHByb2R1Y2UgdGhlIHZpcnVzIGFuZCBzcHJlYWQgaXQgdG8gb3RoZXJzLsKg[Qq]
[q multiple_choice=”true”] True or false: if you can still taste or smell, you aren’t infected with SARS-CoV-2
[c]IFRydWU=[Qq]
[f]IE5vLiBXaGlsZSBtb3N0IHBlb3BsZSB3aG8gaGF2ZSBiZWNvbWUgaW5mZWN0ZWQgd2l0aCBTQVJTLUNvVi0yIGV4cGVyaWVuY2UgbG9zcyBvZiB0YXN0ZSBvciBzbWVsbCwgaXQmIzgyMTc7cyBub3QgYSBzdXJlIHRoaW5nLsKgSW4gb3RoZXIgd29yZHMsIHlvdXIgc2Vuc2Ugb2YgdGFzdGUgYW5kIHNtZWxsIGNhbiBiZSBmaW5lLCBhbmQgeW91IGNhbiBzdGlsbCBiZSBpbmZlY3RlZC4gVGhhdCYjODIxNztzIHdoeSBpdCYjODIxNztzIGltcG9ydGFudCB0byBtYWludGFpbiBzb2NpYWwgZGlzdGFuY2UgYW5kIHRvIHdlYXIgYSBtYXNrIHdoZW4gYXJvdW5kIG90aGVycy7CoA==[Qq]
[c]IEZh bHNl[Qq]
[f]IFRoYXQmIzgyMTc7cyBjb3JyZWN0LsKgV2hpbGUgbW9zdCBwZW9wbGUgd2hvIGhhdmUgYmVjb21lIGluZmVjdGVkIHdpdGggU0FSUy1Db1YtMiBleHBlcmllbmNlIGxvc3Mgb2YgdGFzdGUgb3Igc21lbGwsIGl0JiM4MjE3O3Mgbm90IGEgc3VyZSB0aGluZy4gSW4gb3RoZXIgd29yZHMsIHlvdXIgc2Vuc2Ugb2YgdGFzdGUgYW5kIHNtZWxsIGNhbiBiZSBmaW5lLCBhbmQgeW91IGNhbiBzdGlsbCBiZSBpbmZlY3RlZC7CoA==[Qq]
[q] A big problem experienced during COVID-19 is that an infected person’s immune system might react to the infection in a way that causes too much [hangman]. This causes fluid and pus to build up in the lungs, making it hard for someone to absorb enough [hangman].
[c]IGluZmxhbW1hdGlvbg==[Qq]
[f]IEV4Y2VsbGVudCE=[Qq]
[c]IG94eWdlbg==[Qq]
[f]IEV4Y2VsbGVudCE=[Qq]
[q] One goal of a vaccine is to get your [hangman] system to produce [hangman] cells. These cells enable your body to quickly respond to and fight off an infection.
[c]IGltbXVuZQ==[Qq]
[f]IEdyZWF0IQ==[Qq]
[c]IG1lbW9yeQ==[Qq]
[f]IEdyZWF0IQ==[Qq]
[q] Two vaccines that have been developed to fight COVID-19 both use the nucleic acid [hangman], enclosed within a(n) [hangman] envelope.
[c]IFJOQQ==[Qq]
[f]IEdvb2Qh[Qq]
[c]IGxpcGlk[Qq]
[f]IEdvb2Qh[Qq]
[q] The big idea behind mRNA vaccines is that they get your cells to produce SARS-CoV-2’s [hangman] protein (as shown in A and J). This enables your immune system to produce [hangman] to the virus (shown at K), enabling you to fight off subsequent infections.
[c]IHNwaWtl[Qq]
[f]IEV4Y2VsbGVudCE=[Qq]
[c]IGFudGlib2RpZXM=[Qq]
[f]IENvcnJlY3Qh[Qq]
[q] In the diagram below, mRNA coding for the spike protein is shown at
[textentry single_char=”true”]
[c]IE I=[Qq]
[f]IEV4Y2VsbGVudDogbVJOQSBmb3IgdGhlIHNwaWtlIHByb3RlaW4gaXMgc2hvd24gYXQgJiM4MjIwO0IuJiM4MjIxOw==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBtUk5BIGlzIGEgc2luZ2xlLXN0cmFuZGVkIG51Y2xlaWMgYWNpZC4=[Qq]
[q] The goal of an mRNA vaccine is to get human cells to produce a viral protein, leading to the development of an immune response. In the diagram below, that human-produced viral protein is indicated by which letter?
[textentry single_char=”true”]
[c]IE o=[Qq]
[f]IE5pY2Ugam9iLiBBIGh1bWFuLXByb2R1Y2VkIHZpcmFsIHByb3RlaW4gaXMgc2hvd24gYXQgJiM4MjIwO0ouJiM4MjIxOw==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGVyZSYjODIxNztzIG9ubHkgb25lIHBsYWNlIGluIHRoZSBkaWFncmFtIHdoZXJlIHlvdSBzZWUgcHJvdGVpbiBzeW50aGVzaXMuIEZpbmQgdGhhdCBwbGFjZSwgYW5kIGl0JiM4MjE3O3Mgb25lIG9mIHRoZSBsZXR0ZXJzIGluIHRoYXQgcGFydCBvZiB0aGUgZGlhZ3JhbS4=[Qq]
[q] In the diagram below, the vaccine is shown fusing with a human cell at
[textentry single_char=”true”]
[c]IE g=[Qq]
[f]IEF3ZXNvbWUuIEggc2hvd3MgdGhlIHZhY2NpbmUgZnVzaW5nIHdpdGggYSBodW1hbiBjZWxsLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGlzIGZ1c2lvbiBiZXR3ZWVuIHRoZSB2YWNjaW5lIGFuZCBhIGh1bWFuIGNlbGwgbG9va3MgYSBiaXQgbGlrZSB0d28gc29hcCBidWJibGVzIGpvaW5pbmcgdG9nZXRoZXIu[Qq]
[q] In the diagram below, the lipid envelope that protects the injected mRNA when it’s in the bloodstream and which lets it get into a human cell is indicated by which letter?
[textentry single_char=”true”]
[c]IE U=[Qq]
[f]IEdvb2Qgd29yay4gTGV0dGVyICYjODIyMDtFJiM4MjIxOyBpcyB0aGUgbGlwaWQgZW52ZWxvcGUgdGhhdCBwcm90ZWN0cyB0aGUgbVJOQSBhbmQgd2hpY2ggbGV0cyBpdCBnZXQgaW50byBhIGh1bWFuIGNlbGwu[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGUgbGlwaWQgZW52ZWxvcGUgc3Vycm91bmRzIHRoZSBtUk5BLg==[Qq]
[q] The goal of an mRNA vaccine is to get the immune system to produce antibodies to the virus. In the diagram below, these antibodies are shown at
[textentry single_char=”true”]
[c]IE s=[Qq]
[f]IEF3ZXNvbWUuIEFudGlib2RpZXMgdG8gdGhlIHZpcnVzIGFyZSBzaG93biBhdCBLLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBMb29rIGZvciBzb21ldGhpbmcgdGhhdCBzZWVtcyB0byBiZSByZXNwb25kaW5nIG9yIHJlYWN0aW5nIHRvIHRoZSBodW1hbi1wcm9kdWNlZCBzcGlrZSBwcm90ZWluIGF0ICYjODIyMDtKLiYjODIyMTs=[Qq]
[q] In the diagram below, a human ribosome is reading viral mRNA, producing a viral protein. That ribosome is shown at
[textentry single_char=”true”]
[c]IE k=[Qq]
[f]IEdvb2Qgd29yay4gJiM4MjIwO0kmIzgyMjE7IHNob3dzIGEgaHVtYW4gcmlib3NvbWUgcmVhZGluZyB2aXJhbCBtUk5BLg==[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBSaWJvc29tZXMgJiM4MjIwO3JlYWQmIzgyMjE7IG1STkEsIHByb2R1Y2luZyBwcm90ZWlucy4gRmluZCB0aGUgdmlyYWwgbVJOQSBpbnNpZGUgYSBodW1hbiBjZWxsLCBhbmQgeW91JiM4MjE3O2xsIGZpbmQgdGhlIGFuc3dlci4=[Qq]
[q] In the diagram below, a long string of repeated adenine nucleotides that protects the mRNA from enzymatic breakdown is shown at
[textentry single_char=”true”]
[c]IE Q=[Qq]
[f]IE5pY2Ugd29yay4gTGV0dGVyICYjODIyMDtEJiM4MjIxOyBzaG93cyB0aGUgcG9seS1BIHRhaWwsIGEgc3RyaW5nIG9mIHJlcGVhdGVkIGFkZW5pbmUgbnVjbGVvdGlkZXMgdGhhdCBwcm90ZWN0cyB0aGUgbVJOQSBmcm9tIGVuenltYXRpYyBhdHRhY2su[Qq]
[c]IEVudGVyIHdvcmQ=[Qq]
[c]ICo=[Qq]
[f]IE5vLiBIZXJlJiM4MjE3O3MgYSBoaW50LiBUaGlzIHBhcnQgb2YgdGhlIG1STkEgaXMgY2FsbGVkIGEgcG9seS1BIHRhaWwuIFdoYXQgb24gdGhlIGRpYWdyYW0gY291bGQgYmUgY2FsbGVkICYjODIyMDtwb2x5LUE/JiM4MjIxOw==[Qq]
[q]The diagram below shows a SARS-CoV-2 particle that’s been [hangman]. That’s because the [hangman] covering the spike proteins will keep the virus from [hangman] any more cells.
[c]bmV1dHJhbGl6ZWQ=[Qq]
[c]YW50aWJvZGllcw==[Qq]
[c]aW5mZWN0aW5n[Qq]
[/qwiz]
10. Staying Safe
Getting vaccinated is the best way to avoid SARS-CoV-2 infection and serious COVID-19 disease. While some vaccinated people have experienced breakthrough infections, the severity of their symptoms is significantly less than what they would have experienced if they hadn’t been vaccinated. Vaccination also reduces your potential to spread the virus. If you haven’t been vaccinated, I hope that the information above might sway you to make a different decision.
In terms of other protective measures, I don’t have anything new to say about how to avoid infecting others or becoming infected yourself, so I’ll repeat what’s widely known.
- When it’s necessary, wear a mask
- N95s provide the best protection. Surgical masks provide less protection, and cloth masks even less.
- To avoid infection, wear one whenever you’re inside, in a public space.
- Wear one when you’re around others whose infection status is unknown.
- Know your infection status. Rapid antigen tests are available at any pharmacy, and many institutions provide them for free. If you have a concern about your infection status, test yourself so that you can avoid infecting others.
- Maintain distance. The closer you are to someone else who’s infected, the higher the concentration of the virus that you’ll breathe in. The reverse would be true if you were infected. If you don’t know others’ infection status, then keep your distance to avoid spreading the virus.
- Ventilate your space: If you are working indoors in the presence of others, wear a mask, and keep the room that you’re in well-ventilated.
What’s Next
- There’s one tutorial left in this module. Please use the following link to learn about Rapid Antigen Testing for COVID-19.
- Please use this link for more resources about SARS-CoV-2 and COVID-19.
